June 2023 | VOL. 22, NO. 6| www.McGowan.pitt.edu
Stories by Cristina D’Imperio
“He was brilliant.” Obituary: John N. Murphy

Professor John N. Murphy, McGowan’s first executive director, passed away on June 13, 2023, from complications related to Parkinson’s Disease. He was 83.
A pioneering scientist and engineer, as well as a devoted father and husband, Prof. Murphy’s work helped advance Pittsburgh’s prominence in the global scientific community.
Whether he was working as Director of the Pittsburgh Research Center of the U.S. Bureau of Mine Safety, collaborating with NASA on propulsion systems for manned space travel, teaching in the classroom at the University of Pittsburgh, or in a leadership role at the McGowan Institute, “he was inseparable from the work he was doing and the impact he was having,” stated his son Michael Murphy in an interview with the Pittsburgh Post-Gazette. “He really believed in it, and it was the most important thing.”
Prof. Murphy’s passion for the work he was doing extended, too, to volunteering. For instance, when his son became a Boy Scout, Prof. Murphy not only became an assistant scoutmaster and later a committee chair, he also wrote his own merit badge – Mining in Society. The badge teaches about the role mining has had in history and how it continues to impact daily life.
According to his son, one of Prof. Murphy’s favorite phrases was “Silence is the better part of valor.” He believed that listening and serving were more important than speaking. “He was very giving of himself and his time. He always put himself behind other people and they were attracted to him because of that humility. They recognized how smart he really was when he came to the table with zero pretense.” Put simply, “He was brilliant.”
Prof. Murphy’ legacy of innovation, leadership, mentorship, and passion for his work will be carried on at the McGowan Institute.
He is survived by his wife Catherine, son Michael, brothers Thomas and Richard, and three grandchildren.
The full obituary in the Pittsburgh Post-Gazette can be found here.
RESOURCES AT THE MCGOWAN INSTITUTE
July Histology Special – TUNEL Assay
Apoptosis, or “programmed cell death”, is a form of cell death designed to eliminate compromised or senescent cells. Apoptosis is controlled by multiple signaling and effector pathways that in turn, are activated in response to external growth, survival, or death factors.
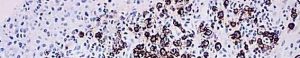
The McGowan Histology Core offers TUNEL staining on paraffin embedded or frozen tissue.
You’ll receive 30% off TUNEL staining in July when you mention this ad.
Contact Julia at the McGowan Core Histology Lab by email: Hartj5@upmc.edu or call 412-624-5265.
Sample Submission Procedures: Please contact us to schedule a drop off time. When you arrive at the building you can call our laboratory at (412) 624-5365. Someone will meet you in the lobby to collect your samples. When your samples are completed, you will receive an email to schedule a pickup time.
SCIENTIFIC ADVANCES
Drs. Sanchez, Gerlach, and Noda Awarded R21 Funding

Pablo G. Sanchez, MD, PhD, (pictured center) McGowan affiliated faculty and Chief, Division of Lung Transplant and Lung Failure in the Department of Cardiothoracic Surgery at the University of Pittsburgh, as well as Brack G. Hattler Professor in Cardiothoracic Transplantation, and Jörg C. Gerlach, MD, PhD, (pictured right) Director of the interdisciplinary Biorector Group at the McGowan Institute, are the Principal Investigators (PIs) on a new R21 award from the National Heart, Lung, and Blood Institute. Kentaro Noda, PhD, (pictured left)Research Program Manager of Ex Vivo Lung Perfusion in the Department of Cardiothoracic Surgery at the University of Pittsburgh is also part of the project.
The project, titled “Incorporating hepatic cell function into lung ex vivo lung perfusion for transplant preservation” spans from April 2023 to January 2025.
The project aims “to provide proof-of-principle for the ability of hepatocyte BRx to enhance lung graft preservation.” Lung graft preservation, conducted with static cold storage, is limited to 8 hours or less. The longer an organ remains in cold storage, the chances of primary graft dysfunction increases.
According to the project abstract:
[P]rimary graft dysfunction is a risk factor for developing chronic rejection, which could account for the low 5-year survival rate (50%) following lung transplantation (LTx). Ex Vivo Lung Perfusion (EVLP) is expected to improve lung preservation and transplant outcomes by providing normothermic circulation and ventilation. A problem is that current EVLP is self-limited by normothermia-activated lung metabolism. The accumulation of toxic metabolites leads to a proinflammatory state, activating Receptor of Advanced Glycation End-Products (RAGE) and nuclear factor (NF)-kB mechanisms, which in turn upregulate proinflammatory cytokine signaling. […] In previous work, we have maintained normal hepatic detoxification, synthesis, and regulation in in vitro circuits using liver cell bioreactors (BRx). […] We will incorporate a hepatic BRx in our established EVLP circuits and demonstrate its effect on short-term LTx in experimental rat models. We will repeat these experiments using a cadaveric human EVLP model. We will conduct comprehensive phenotypic, transcriptional, and functional endpoint assessments on lung tissue and hepatic cells in BRx, such as RAGE and NF-kB.
The project seeks to change the current state of EVLP for lung preservation in order to permit lungs to be preserved for longer periods of time outside of the donor body with less damage to the organ. This equates to increasing viable donor organ transportation time and distance, improving lung transplant wait lists, and ultimately improving post-transplant patient survival.
Dr. Robert Kormos Announces Two New FDA Clearances

Robert L. Kormos, MD, (pictured) McGowan affiliated faculty and the Division Vice President Global Medical Affairs Heart Failure at Abbott Laboratories in Austin, Texas, is part of an announcement from Abbott about two new clearances from the U.S. Food and Drug Administration (FDA).
Abbott’s CentriMag Blood Pump can now be used to provide longer-term life support for critically ill patients, and its CentriMag Pre-connected Pack has received FDA clearance for life support lasting less than six hours. Both devices provide physicians with more time to make critical care decisions.
The pump temporarily replaces the function of the heart and has been used to treat patients with COVID-19 as well as those who have had heart surgery and others for whom extracorporeal membrane oxygenation (ECMO) is critical to saving their life.
The preconnected pack provides urgent cardiopulmonary support by combining system components including the oxygenator and the blood pump. Previously, physicians needed to put the system together from separate components.
Dr. Kormos stated, “With CentriMag, our mission has always been to transform the treatment of advanced cardiac and respiratory conditions to improve clinicians’ ability to most effectively manage their sickest patients. With the two new FDA clearances, physicians can deploy support in fewer steps and are provided more time to get their patients the necessary treatment during a critical window.”
Read the full press release here.
Collaboration and Partial Liver Transplants Key in Preventing Pediatric Waitlist Deaths
 George V. Mazariegos, MD, McGowan affiliated faculty and the Director of the Hillman Center for Pediatric Transplantation at the Children’s Hospital of Pittsburgh of UPMC, is the lead author of a study published in the July 2023 issue of Liver Transplantation.
George V. Mazariegos, MD, McGowan affiliated faculty and the Director of the Hillman Center for Pediatric Transplantation at the Children’s Hospital of Pittsburgh of UPMC, is the lead author of a study published in the July 2023 issue of Liver Transplantation.
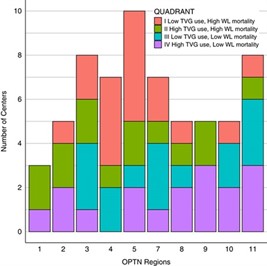
The article, titled “Center use of technical variant grafts varies widely and impacts pediatric liver transplant waitlist and recipient outcomes in the United States,” assesses the impact of technical variant grafts (TVGs), including living donor and deceased donor split/partial grafts, on waitlist and transplant outcomes for pediatric liver transplant candidates.
The research suggests that greater use of partial liver transplants could help save the lives of children on liver transplant waitlists. The study found that medical facilities offering TVGs had fewer waitlist deaths than those providing whole deceased donor liver transplants only.
“Since the first successful liver transplant in Pittsburgh 42 years ago, we’ve made tremendous advances, but significant gaps still remain nationally,” said Dr. Mazariegos. “It’s tragic that 6% of children are still dying on the liver transplant waitlist in the United States. The goal is zero.”
More training, support, and collaboration between medical facilities on TVG transplants could help to eliminate pediatric waitlist mortality.
“We need more training and support to develop technical variant graft programs and expertise at transplant centers across the country,” said Dr. Mazariegos. “At the end of the day, it’s about every center committing to giving every child the best opportunity to receive and thrive after their transplant. I strongly believe that the way forward is collaboration, not competition.”
Dr. Mazariegos maintained that pediatric liver transplant waitlist mortality “is a solvable problem, and we can fix it today if we work together to identify critical challenges and best practices.”
New Approach to Treating Chronic Transplant Rejection

Anthony J. Demetris, MD, McGowan affiliated faculty and Endowed Chair at the Starzl Professor of Liver and Transplant Pathology in the Department of Pathology at the University of Pittsburgh, recently co-authored a study in Science Immunology titled “Tissue-resident memory T cell maintenance during antigen persistence requires both cognate antigen and interleukin-15.”
The study points to a new approach to treating chronic transplant rejection. Dr. Demetris, alongside lead author Roger Tieu, PhD, and other co-authors, identified a type of immune cell that drives chronic organ transplant failure in mice. According to the paper’s abstract, their findings, “provide insights that could lead to improved treatment of chronic transplant rejection and autoimmunity.”
Fadi Lakkis, MD, co-senior author of the study and Scientific Director of the Starzl Transplantation Institute at the University of Pittsburgh, states, “In solid organ transplantation, such as kidney transplants, one-year outcomes are excellent because we have immunosuppressant drugs that manage the problem of acute rejection.”
However, Dr. Lakkis continues, “Over time, these organs often start to fail because of a slower form of rejection called chronic rejection, and current medications don’t seem to help. Understanding this problem was the motivation behind our study.”
The researchers hope that their findings are the precursors to clinical trials in transplant patients. “In my medical school training,” says Tieu, “I have had the privilege of working with transplant patients. I am excited that our work has the potential to be translated from lab to clinic, with the goal of mitigating chronic rejection and elevating quality of life for our patients.”
Science Immunology image credit Ella Maru Studio.
Dr. Webster-Wood to Lead Transdisciplinary Team Building Actuators for Bio-bots

Victoria Webster-Wood, PhD, (pictured) McGowan affiliated faculty and Assistant Professor in Mechanical Engineering at the University of Pittsburgh with a courtesy appointment in Biomedical Engineering at Carnegie Mellon University (CMU), will head a team of researchers from CMU, Northwestern University, and The Georgia Institute of Technology.
The team received a $6.25 million Multidisciplinary University Research Initiative (MURI) grant from the Department of Defense (DOD).
Comprised of researchers in biomedical engineering, mechanical engineering, electrical engineering, and computer science, the transdisciplinary team will study issues in biohybrid systems.
According to a press release, “the project aims to identify how to combine living materials, protein-based materials and engineered materials to build larger scale, self-sustaining bio-actuators; understand how to keep these materials alive in a real-world environment; and determine how to leverage computational design strategies to improve peak performance.”
As founder and director of CMU’s Biohybrid and Organic Robotics Group (BORG), Dr. Webster-Wood is interested in connections between animals and robotics. Animals have long served as an inspiration for robotics; however, many of the mechanical properties, physical capabilities, and the behavioral flexibility seen in animals have yet to be achieved in robotic platforms. Towards addressing this gap, the BORG’s research focuses on the use of organic materials as structures, actuators, sensors, and controllers toward the development of biohybrid and organic robots and biohybrid prosthetics.
“Right now our biohybrid robots run around in petri dishes and in sterile incubators,” explains Dr. Webster-Wood. “Through this project we hope to leverage our understanding of living muscle to create stronger, more useful muscle-based actuators.”
The research group’s long-term goal is to develop completely organic, autonomous robots with programmable neural circuits. Such robotic systems will have applications in search and rescue, environmental monitoring, and prosthetics. Biohybrid actuators will make it possible for the robots to “grow, develop, and heal as they operate in the real world.”
“This research lays the foundation to move these actuators to translation,” notes Dr. Webster-Wood. “We hope to get living muscle-based actuators to the point where they are reliable and predictable enough that someone can select one, just like they would a motor, and put them to use in a robot.”
Image credit: Carnegie Mellon University News, May 3, 2023.
From Ice Hockey to Studying Heart Valves at the Wagner Lab

In the Wagner Cardiovascular Engineering Lab at the McGowan Institute, University of Pittsburgh student Benjamin Leslie (pictured) studies congenital heart defect (CHD) valve malformations that can result in heart or valve infections, irregular heartbeats, blot clots, heart failure, and strokes.
In between his time at the lab and juggling 18-credit semesters, Leslie is a forward on Pitt’s Division 1 men’s ice hockey team. In 2023, the team won the season’s Eastern States Collegiate Hockey League tournament and achieved its highest ranking in program history, coming in at No. 9. To date, Leslie’s hockey career spans more than 91 games.
In fact, it’s his love of ice hockey that’s spurred his passion in the lab. Leslie is especially interested in children experiencing the symptoms of CHD valve malformations. Each year, approximately 40,000 babies are born with CHD.
“For these kids, childhood often means a lot of time in the hospital undergoing major cardiac procedures,” Leslie said. “When I was a kid, I wanted to have fun and run around with my friends. To not to be able to enjoy any high-intensity activity or sport, let alone hockey, I can’t imagine how awful that must be.”
Current treatments include valve replacements, surgical procedures, and medications. However, each of these can have serious side effects.
At the Wagner Lab, Leslie has become intrigued by cellular engineering and studies valves made from the patient’s own tissues. The valves can grow as the patient does, reducing the number of surgeries the patient might need.
“Additionally, by being made from the patient’s own cells, the need for blood thinners would not be required,” said Leslie. “Therefore, children would be able to partake in sports like every other kid, without the risk of bleeding. This could give every kid a chance.”
Leslie’s drive is evident on and off the ice. On the ice, he’s known as a team captain, for his quick shot, and leading by example. Off the ice and in the lab, doctoral bioengineering student Drake Pedersen, who supervises Leslie, stated, “His eagerness to learn about the impact of our research was indicative of the type of student I appreciate training.”
The futures of both Leslie and tissue engineering look promising. And, while Leslie is still deciding on his plans as he enters his senior year at Pitt, Pedersen noted, “I’m not sure where Ben’s path will take him, but I feel he will excel wherever he goes.”
Image courtesy of Pitt Athletics.
McGowan in the News: Growing Pennsylvania’s “Space Ecosystem”

From June 1-2, 2023, the second annual Keystone Space Conference was held in Pittsburgh. The conference is part of the Keystone Space Collaborative, a non-profit whose mission is to support the space industry in Pennsylvania, Ohio, and West Virginia by making commercial space opportunities more accessible, as well as attracting space industry businesses and talent to the tri-state area.
At the conference, Department of Community and Economic Development Secretary (DCED) Rick Siger announced that the Shapiro Administration made new investments to boost Pennsylvania’s leadership in the aerospace sector.
“The Shapiro Administration is thrilled to support Pennsylvania’s growing space industry,” said Secretary Siger. “The Commonwealth’s diverse space ecosystem is rooted in a legacy of innovation and is supported by a highly educated workforce and world-class research institutions. We look forward to building on Pennsylvania’s success, and ensuring our companies continue to lead the way in this dynamic sector.”
McGowan’s microgravity biotech commercialization research was specifically highlighted as part of Pennsylvania’s “legacy of innovation.” The McGowan Institute was also mentioned as one of the area’s key research institutes crucial to “fueling the research and workforce that space companies need to succeed […] and ensuring that the rapidly accelerating growth in this sector is collaborative, inclusive, and strategic.”
AWARDS AND RECOGNITION
Dr. Paul Monga Becomes Director of the New Pittsburgh Liver Institute

Dr. Satdarshan (Paul) Monga, Director of McGowan’s Cellular Approaches to Tissue Engineering and Regeneration (CATER) Training Program and Endowed Chair for Experimental Pathology at the University of Pittsburgh, has been appointed director of the new Pittsburgh Liver Institute (PLI).
Dr. Monga has served as founding director of the Pittsburgh Liver Research Center (PLCR) since 2016. “The PLRC bridges the intellectual exchange between clinicians and researchers in the hope of improving the clinical care of liver patients,” states Dr. Monga. “Specifically, the PLRC supplies research funding, scientific core facilities, unique scientific and clinical resources, networking and collaborations, mentoring, and enrichment programs in the areas of liver regenerative medicine, liver diseases, and liver tumors.”
The PLI will house the PLRC and will be a broader, financially independent institute geared toward developing additional liver-focused initiatives and programs, training grants and public outreach activities. As part of its key objectives, the PLI will form multidisciplinary and interdisciplinary research teams, international collaborations and industry partnerships, and also serve as a specialized liver-medicine training hub.
Through research, training, and translation, the PLI aims to transform Pittsburgh into the “liver corridor” of the world.
Dr. Rory Cooper Receives Distinguished Eagle Scout Award

The Distinguished Eagle Scout Award (DESA) is the National Eagle Scout Association’s (NESA’s) highest honor. It is presented to Eagle Scouts who have achieved “extraordinary national-level recognition, fame, or eminence within their profession and/or service to the nation and have a strong record of voluntary service to their community.” Fewer than five people receive the award each year.
Rory Cooper, PhD, McGowan affiliated faculty, was recently awarded the Distinguished Eagle Scout Award. Dr. Cooper is a Paralympian, Army veteran, inventor, engineer, and disability advocate. He is also the Founding Director and VA Senior Research Career Scientist of the Human Engineering Research Laboratories, a collaboration between the University of Pittsburgh and the U.S. Department of Veterans Affairs Office of Research and Development.
Strict award criteria include a minimum of 25 years “Time in Service” from the date the Eagle rank was achieved. Dr. Cooper is the only person from Western Pennsylvania to have received the award in the past 15 years.
The award was first introduced in 1969, and previous recipients include former President Gerald R. Ford, director Steven Spielberg, and astronaut Neil Armstrong.
Congratulations, Dr. Cooper!
Dr. Anne Robertson Delivers Elsevier Distinguished Lecture at Berkeley

Anne Robertson, PhD, (pictured) McGowan affiliated faculty and Distinguished Service Professor and William Kepler Whiteford Endowed Professor of Mechanical Engineering and Materials Science at the University of Pittsburgh, was recently selected to give the Elsevier Distinguished Lecture at the University of California, Berkeley.
The Elsevier Distinguished Lecture is an honor given to scientists and researchers who have made significant contributions to their respective fields, specifically those who have demonstrated exceptional research and who have the potential to inspire future generations of scientists.
Dr. Robertson’s research interests include continuum mechanics with an emphasis on cerebral vascular disease, constitutive modeling of soft biological tissues, and non-Newtonian fluid mechanics.
Her lecture, titled “Unraveling the Mechanics of Biological Soft Tissue Using Advanced Bioimaging Techniques,” focused on recent work utilizing advances in bioimaging technology. In particular, Dr. Robertson discussed multiphoton microscopy, a bioimaging tool used for visualizing cellular and subcellular events within living tissue; it allows for direct imaging without fixation or destructive tissue sectioning.
Dr. Robertson further discussed recent work she and her team conducted using multiphoton microscopy to simultaneously image collagen and elastin fiber organization during mechanical experiments. Collagen and elastin fibers, which are found in soft tissues like arteries, the bladder, and cornea, are crucial for enabling specific functions within each. For instance, the study of soft tissues lends itself to a better understanding of the high compliance of the bladder wall, rupture of cerebral aneurysms, and the growth and remodeling in blood vessels.
“Professor Robertson’s research is world-class, with an impact on many fields of study. Her selection is not only well deserved, but it also serves as an inspiration to future generations of female engineers,” said Brian Gleeson, Harry S.Tack Chair Professor and Chair of the Department of Mechanical Engineering and Materials Science. “By recognizing the achievements of individuals like Professor Robertson, we are encouraged to continue to push the boundaries of what is possible.”
Dr. Kozai Presents at Neuroengineering Conference

Takashi Daniel Yoshida Kozai, PhD, McGowan affiliated faculty and Assistant Professor in the Department of Engineering at the University of Pittsburgh was one of 35 presenters at Rice University’s InterfaceRice conference in May.
The event is centered around neuroengineering and is structured as a conversation between engineers, researchers, clinicians, and businesspeople. The conference includes panel discussions on the latest research in the field as well as on topics such as translation, ethics, and government policy.
Dr. Kozai’s session, “Shining Light on the Brain: Advances in Optical Microscopy,” focused on light microscopy as a way to obtain images of neurons and other cells in action. He provided an overview of new advances and experimental capabilities, including functional imaging at faster speeds, greater depths, and over larger tissue volumes.
Dr. Kozai’s research employs in vivo multi-photon microscopy, functionally evoked electrophysiology, post-mortem multi-channel immunohistochemistry, impedance spectroscopy, device design, and emerging biomaterial tools.
The InterFace 2023 Conference Schedule can be found here.
PUBLICATION OF THE MONTH
Author: George V. Mazariegos; Emily R. Perito; James E. Squires; Kyle A. Soltys; Adam D. Griesemer; Sarah A. Taylor; Eric Pahl.
Title: Center use of technical variant grafts varies widely and impacts pediatric liver transplant waitlist and recipient outcomes in the United States
Summary: To assess the impact of technical variant grafts (TVGs) [including living donor (LD) and deceased donor split/partial grafts] on waitlist (WL) and transplant outcomes for pediatric liver transplant (LT) candidates, we performed a retrospective analysis of Organ Procurement and Transplantation Network (OPTN) data on first-time LT or liver-kidney pediatric candidates listed at centers that performed >10 LTs during the study period, 2004–2020. Center variance was plotted for LT volume, TVG usage, and survival. A composite center metric of TVG usage and WL mortality was developed to demonstrate the existing variation and potential for improvement. Sixty-four centers performed 7842 LTs; 657 children died on the WL. Proportions of WL mortality by center ranged from 0% to 31% and those of TVG usage from 0% to 76%. Higher TVG usage, from deceased donor or LD, independently or in combination, significantly correlated with lower WL mortality. In multivariable analyses, death from listing was significantly lower with increased center TVG usage (HR = 0.611, CI: 0.40–0.92) and LT volume (HR = 0.995, CI: 0.99–1.0). Recipients of LD transplants (HR = 0.637, CI: 0.51–0.79) had significantly increased survival from transplant compared with other graft types, and recipients of deceased donor TVGs (HR = 1.066, CI: 0.93–1.22) had statistically similar outcomes compared with whole graft recipients. Increased TVG utilization may decrease WL mortality in the US. Hence, policy and training to increase TVG usage, availability, and expertise are critical.
Source: Liver Transplantation 29(7):p 671-682, July 2023.
GRANT OF THE MONTH
PI: Pablo Sanchez
Co-PI: Joerg Gerlach
Title: Incorporating hepatic cell function into lung ex vivo lung perfusion for transplant preservation
Description: IIn contrast with other organs, preservation times of lung grafts for transplantation are limited to no more than 8 hours with standard cold preservation. Declining quality with extending preservation times increases the risk of primary graft dysfunction, a risk factor for developing chronic rejection, which could account for the low 5-year survival rate (50%) following lung transplantation (LTx). Ex Vivo Lung Perfusion (EVLP) is expected to improve lung preservation and transplant outcomes by providing normothermic circulation and ventilation. A problem is that current EVLP is self-limited by normothermia-activated lung metabolism. The accumulation of toxic metabolites leads to a proinflammatory state, activating Receptor of Advanced Glycation End-Products (RAGE) and nuclear factor (NF)-κB mechanisms, which in turn upregulate proinflammatory cytokine signaling. Experimentally, cross-circulation of a whole swine with EVLP by others demonstrated improved lung resuscitation, but the exact contributors to this improvement remain unclear. Own in vitro preliminary data suggest a role for hepatic function in enhancing endothelial preservation. In previous work, we have maintained normal hepatic detoxification, synthesis, and regulation in in vitro circuits using liver cell bioreactors (BRx). We hypothesize first that the liver function in the swine cross-circulation model played a major role in enhancing EVLP and tissue viability. We also hypothesize that a hepatocyte BRx can partly substitute for whole-swine liver function on EVLP and maintain the observed improvements lung preservation and LTx outcomes. Our Specific Aim is to provide proof-of-principle for the ability of hepatocyte BRx to enhance lung graft preservation. We will incorporate a hepatic BRx in our established EVLP circuits and demonstrate its effect on short-term LTx in experimental rat models. We will repeat these experiments using a cadaveric human EVLP model. We will conduct comprehensive phenotypic, transcriptional, and functional endpoint assessments on lung tissue and hepatic cells in BRx, such as RAGE and NF-κB. If successful, our technology will provide the means to change the current state of EVLP for lung preservation and allow lungs to be maintained longer outside the donor body with less cellular injury. Ultimately, our work will address current limitations in LTx, including increasing viable donor organ transportation time and distance, helping reduce LTx waiting lists, and improving post-transplant patient survival.
Source: National Heart, Lung, and Blood Institute
Term: April 1, 2023 – January 31, 2025
Amount: $238,500
