May 2023 | VOL. 22, NO. 5| www.McGowan.pitt.edu
Stories by Cristina D’Imperio
The “Heart and Soul” of the McGowan Institute: Executive Director John Murphy Retires

“You only get out of it what you put into it.” In a 2015 interview with the Oral History Center at the University of California, Berkeley, Professor John N. Murphy (pictured) spoke on topics related to his career, including his tenure at the U.S. Bureau of Mines, the University of Pittsburgh, and the McGowan Institute for Regenerative Medicine.
On local, national, and international levels, Professor Murphy’s career exemplifies the hard work, knowledge, and dedication those words imply.
Fresh out of the University of Pittsburgh in 1961 after earning a Bachelor of Science in Engineering, Prof. Murphy became employed as an Electrical Research Engineer at the U.S. Bureau of Mines, working primarily to ensure greater mine safety. By 1978, he was the Director of the Pittsburgh Research Center of the Bureau, and with a team of 350 people, collaborated with mining bodies around the world to promote and enhance the health and safety of miners globally. Many of his projects included ways to prevent and minimize the consequences of fires and explosions in underground and surface mines. Prof. Murphy further worked to develop micro-ventilation circuits. These helped to suppress dust generation and exposure to dust, allowing miners to breathe more safely¾and are still in use today.
While at the Bureau, Prof. Murphy also completed work for every federal agency, including the Department of Defense, the Department of Transportation, and the National Aeronautics and Space Administration (NASA).
Collaborating with NASA during an era when space exploration captivated the world, Prof. Murphy was part of a team that evaluated the destruct system for the new rocket, Titan II. Titan II was used as the propulsion system for NASA’s Gemini program of both uncrewed launches and two-person crewed space capsules. Every launch was successful.
In the late 1990s, when the Bureau of Mines was absorbed into various other governmental organizations, such as the Department of Energy and the National Institute for Occupational Safety & Health (NIOSH), Prof. Murphy became Senior Scientist at the Pittsburgh lab for NIOSH. It was then that he also began his career at the University of Pittsburgh in the Department of Chemical and Petroleum Engineering.
Within his first few years at the University of Pittsburgh, Prof. Murphy was integral in the design of a new interactive classroom. At the time, it was the first of its kind in Pittsburgh and much of the nation. The classroom emphasized the necessity of teamwork in engineering and had computer-facilitated stations that gave groups of students the ability to present work to the entire class. It’s a design that has now been replicated dozens of times across the country and for which Prof. Murphy has won awards.
It is difficult, however, to convince Prof. Murphy to speak of his awards and accolades. In conversation, he’ll frequently deflect to other topics, including the accomplishments of students and colleagues. Dr. William Wagner, Director of the McGowan Institute, has worked with Prof. Murphy for over 20 years and notes, “John is passionate about seeing his colleagues recognized for their work. He was behind so many nominations of McGowan faculty for international awards and recognitions and delighted in seeing others receive accolades.”
Prof. Murphy’s own awards include the Department of Interior Distinguished Service Award, the Presidential Rank Award for Meritorious Executive, and the Presidential Award for Distinguished Executive among many others. He also holds two patents, has authored more than 90 technical publications, and has served as president and member of various professional and non-profit organizations, including the SME Foundation, the National Mine Rescue Association, and the Institute of Electrical and Electronics Engineers.
In 2001, Prof. Murphy was invited to be the first Executive Director of the McGowan Institute for Regenerative Medicine. What started out as a small group of 25 scientists who were primarily interested in artificial organ technology, has now grown to a group of more than 250 affiliated faculty members across 36 disciplines.
Prof. Murphy holds an MBA from Duquesne University and is as renowned for his management capabilities as he is for his engineering and technological awards and achievements. When asked about his management style, Prof. Murphy explains, “I typically tried to manage by exception. It’s important to delegate and to empower people to do what they think is relevant and important.” Prof. Harvey Borovetz, Deputy Director of Artificial Organs and Medical Devices at the McGowan Institute, has worked with Prof. Murphy for over 20 years. He states, “Professor Murphy’s management style is one I always tried to emulate. He knew what needed to be done and who was responsible for doing it, but he was always kind and helpful even under the tightest deadlines. The heartfelt outpouring from everyone associated with McGowan regarding his retirement is the best evidence I can provide about how deeply appreciated and highly regarded John Murphy is by all of us.”
It is difficult to capture in words the magnitude of what Prof. Murphy has accomplished in his career, not just in terms of his contributions to science and technology, but in terms of the people he’s positively impacted. More than one McGowan associate has described Prof. Murphy as the “heart and soul” of the institute, and Dr. Wagner has called his dedication “legendary.”
When looking back over Prof. Murphy’s tenure as Executive Director, perhaps his own words summarize it best: “It has been an exciting ride.”
Thank you, Prof. Murphy, for your legacy of innovation, leadership, mentorship, and dedication. You put your all into it. And our minds – and hearts – are better for it.
RESOURCES AT THE MCGOWAN INSTITUTE
June Histology Special – Toluidine Blue
Mast cells play a key role in the inflammatory process.
A mast cell is a myeloid derived cell and is part of the immune system. Mast cells contain distinctive granules rich in histamine and heparin. Although best known for their role in allergy and anaphylaxis, mast cells play an important protective role as well, being intimately involved in angiogenesis, defense against pathogens, and wound healing.
Toluidine blue is one of the most common stains for acid mucopolysaccharides and glycoaminoglycans, both of which are components of mast cells granules.
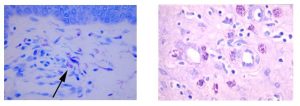
You’ll receive 25% off Toluidine Blue Staining for the entire month on June when you mention this ad.
Contact Julia at the McGowan Core Histology Lab by email: Hartj5@upmc.edu or call 412-624-5265.
Sample Submission Procedures: Please contact us to schedule a drop off time. When you arrive at the building you can call our laboratory at (412) 624-5365. Someone will meet you in the lobby to collect your samples. When your samples are completed, you will receive an email to schedule a pickup time.
SCIENTIFIC ADVANCES
Dr. Chandan Sen and Team to Join the McGowan Institute

Chandan Sen, PhD, MD (pictured), will join the McGowan Institute for Regenerative Medicine, the University of Pittsburgh School of Medicine, and UPMC this summer. Dr. Sen and his team of more than two dozen faculty, postdoctoral associates, and staff are coming to Pittsburgh from Indiana University.
Dr. Sen’s research focuses on developing therapies for chronic wounds, a potentially life-threatening condition that affects millions of people in the U.S. In patients with diabetes, foot ulcers are a common chronic wound with high amputation rates. Sen serves as the special projects chair of the Diabetic Foot Consortium, a multi-center, National Institutes of Health-funded network that aims to improve diabetic wound healing and prevent amputations among the 27 million adults in the U.S. who live with diabetes.
Dr. Sen, a renowned expert in regenerative medicine and pioneer of novel wound care technologies, is known for the development of innovative nanotransfection technology that transforms skin tissue into other types of tissue, which can then be used for healing burns, treating injuries, replacing damaged or diseased tissues, and other therapies.
“Our entire incoming team is excited about the tremendous opportunity to join the Pitt-UPMC ecosystem, well known for its unmatched strength in fostering transformative advances in interdisciplinary biomedical and clinical research,” said Sen. “The McGowan Institute will be home to the Pennsylvania site of the Diabetic Foot Consortium, and the Joslin Diabetes Center at Harvard will serve as our satellite site. Clinical research across 20 UPMC wound care sites supported by innovative basic science research and industry partnerships will position the McGowan Institute as a national leader in this emergent health care discipline.”
Dr. Sen will join Pitt’s faculty as professor of surgery, with a secondary appointment in the Department of Plastic Surgery. He will also hold leadership roles as associate vice chancellor for life sciences innovation and commercialization and positions of co-director of the McGowan Institute and chief scientific officer of UPMC Wound Healing Services.
Drs. Phillippi, Kaczorowski, and Sanchez Awarded R01 Funding

Julie Phillippi, PhD (pictured top), McGowan faculty and UPMC Pellegrini Chair in Cardiothoracic Surgery and Associate Professor of Cardiothoracic Surgery and Bioengineering, is the Principal Investigator (PI) on a new R01 award from the National Heart, Lung, and Blood Institute (NHLBI).
She is partnering with Amrinder Nain, PhD, from Virginia Tech (MPI) and co-investigators David Kaczorowski, MD (pictured middle), McGowan affiliated faculty and Surgical Director of the Advanced Heart Failure Center of the University of Pittsburgh Medical Center (UPMC) Heart and Vascular Institute (HVI) and Pablo Sanchez, MD, PhD (pictured bottom), McGowan affiliated faculty and Chief, Division of Lung Transplant and Lung Failure in the Department of Cardiothoracic Surgery at the University of Pittsburgh.
The project, titled “Matrix biophysics and pericyte mechanobiology in (patho)physiological angiogenesis,” spans from May 2023 until April 2027.
According to the project abstract:
The long-term arc of this project is expected to engineer vascularization of tissue deficits and advance treatment of microvascular diseases including myocardial infarction, atherosclerosis, pulmonary arterial hypertension, aneurysm, peripheral artery disease, bone repair, volumetric muscle loss, diabetic wounds, and cancer. […] The project’s translational impact will be novel methods of controlling microvascular expansion and regression in diseased, damaged, and engineered tissues.
The project seeks to address global health problems including tissue deficits and injuries that involve microvascular dysfunction which would benefit from innovative approaches to better understand angiogenesis and vessel rarefaction.
New Research on the Role of Matrix-Bound Nanovesicles and Biologic Scaffold Materials in the Management of Rheumatoid Arthritis

Rheumatoid arthritis (RA) affects 7.5 million people globally, approximately 1% of the world’s population. RA is a chronic disease, and currently, there is no known cause or cure. It is characterized by chronic inflammation and the destruction of synovial joints.
Raphael J. Crum (pictured), part of the Badylak Lab research team and a fourth year MD/PhD student in the Cellular and Molecular Pathology program at the University of Pittsburgh School of Medicine, is the lead author of an article titled “Immunomodulatory matrix-bound nanovesicles mitigate acute and chronic pristane-induced rheumatoid arthritis.”
Co-authors of the article include George S. Hussey, PhD, McGowan affiliated faculty and Assistant Professor in the University of Pittsburgh’s School of Medicine, and Stephen F. Badylak, DVM, PhD, MD, Deputy Director of the McGowan Institute and Professor in the University of Pittsburgh’s Department of Surgery.
According to the paper’s abstract:
Disease pathology [of RA] is driven by an imbalance in the ratio of pro-inflammatory vs. anti-inflammatory immune cells, especially macrophages. Modulation of macrophage phenotype, specifically an M1 to M2, pro- to anti-inflammatory transition, can be induced by biologic scaffold materials composed of extracellular matrix (ECM). The ECM-based immunomodulatory effect is thought to be mediated in part through recently identified matrix-bound nanovesicles (MBV) embedded within ECM.
Researchers then delivered isolated MBV via injection to rats with pristane-induced arthritis (PIA). The results of MBV administration were compared to the clinical standard of care, intraperitoneal (i.p.) administration of methotrexate (MTX). The overall results of the study “show that the therapeutic efficacy of MBV is equal to that of MTX for the management of acute and chronic pristane-induced arthritis and, further, this effect is associated with modulation of local synovial macrophages and systemic myeloid populations.”
The article, published in Nature’s Portfolio Series, npj Regenerative Medicine, can be read in its entirety here.
New Findings on Macrophages in ER+ Breast Cancer

Estrogen receptor-positive (ER+) breast cancer accounts for approximately 70% of all breast cancers in women and is the most common type of breast cancer diagnosed today. Despite its prevalence, comparatively little is known about its immunobiology.
Steffi Oesterreich, PhD (pictured), McGowan affiliated faculty and the Shear Family Foundation Chair in Breast Cancer Research Professor and Vice-Chair Department of Pharmacology and Chemical Biology, University of Pittsburgh, is part of a team of researchers who recently published their findings on macrophages in ER+ invasive lobular carcinoma (ILC) and invasive ductal carcinoma (IDC) tumors.
The team’s study, published in Nature Cancer and titled “Immune Landscape in Invasive Ductal and Lobular Breast Cancer Reveals a Divergent Macrophage-Driven Microenvironment,” demonstrates “that macrophages, and not T cells, are the predominant immune cells infiltrating the tumor bed.” The team’s analysis of “cellular neighborhoods revealed an interplay between macrophages and T cells” that ultimately highlights “macrophages as a potential target for ER+ breast cancer.”
These findings suggest that tailored immunotherapies, designed to recognize and eliminate cancer cells, are needed to target ILC and IDC.
Dr. Oesterreich notes, “To improve outcomes for patients with these diseases, we need to identify druggable targets focusing on macrophages. There is a huge lack of macrophage-targeting immunotherapies in development – the vast majority focus on T cells.”
The study is an important step toward developing novel immunotherapies for better patient outcomes.
AWARDS AND RECOGNITION
Dr. Kacey Marra is 2023 ATHENA Award Winner

Kacey Marra, PhD (pictured), McGowan core faculty and Professor in the Departments of Plastic Surgery in the School of Medicine (primary) and Bioengineering in the School of Engineering (secondary) as well as Vice Chair of Research for the Department of Plastic Surgery at the University of Pittsburgh, is the recipient of the 2023 Washington County ATHENA Leadership Award.
Supported by the Washington County Chamber of Commerce and sponsored by Crown Castle, Range Resources, and Ironbridge Wealth Counsel, the ATHENA Leadership Award is in its twentieth year of celebrating and honoring women leaders.
“This award promotes leadership by honoring exceptional individuals in the community who contribute in significant ways to the achievements of women and women’s leadership efforts,” said Jeff Kotula, president of the Washington County Chamber of Commerce.
Dr. Marra’s medical device company, Nerve Repair Technologies, was highlighted at the award ceremony. Nerve Repair Technologies focuses on nerve repair and nerve guide fabrication. Among other innovations, Dr. Marra and her team have developed and patented a nerve guide composed of biodegradable, FDA-approved polymers and bioactive factors that will stimulate axon growth.
Dr. Marra was also honored for mentoring over 300 high school, college, graduate, and medical school students.
Congratulations, Dr. Marra!
Image courtesy of Observer-Reporter.
Dr. Cecelia Yates Receives 2024 ASIP Award

Cecelia C. Yates, PhD (pictured), core faculty at the McGowan Institute for Regenerative Medicine (MIRM), is the recipient of the 2024 ASIP Marilyn G. Farquhar Early Career Award for Exceptional Achievement in the Advancement of Women in Experimental Pathology.
The award recognizes individuals who demonstrate exceptional achievement in the advancement of women experimental pathologists during the early phases of their careers. Achievements include training and mentoring women in experimental pathology, leadership within the field of experimental pathology, service to the community in the promotion of science, innovation in the recruitment and retention of women in experimental pathology, and contributions to the Society.
In its recognition of Dr. Yates’ work, the American Society for Investigative Pathology (ASIP) states:
Dr. Yates is one of the first experimental pathologists in the country to hold a primary appointment in a school of nursing…. Her laboratory has been a resource used by over 30 nurse scientists in learning, training, and collecting data using a cellular and molecular pathology translational approach. Dr. Yates…has shown a great interest in preparing and educating the next generation of researchers and scientific innovators [by mentoring] over 50 scholars, including Junior Faculty, Ph.D. and post-doctoral fellows, residents, nursing, medicine, pharmacy, dental medicine, health and rehabilitation, engineering, pathology scholars, and graduate and undergraduate research students at the University of Pittsburgh and institutions nationally.
Additionally, Dr. Yates participates in the School of Nursing Undergraduate Research Mentorship Program (URMP), and she is the Co-Director of the University of Pittsburgh Clinical and Translational Science Fellowship Program (NIH CTSA-TL1) where she mentors pre- and post-doctoral fellows from over eight disciplines.
Dr. Andrew Duncan, a fellow MIRM core faculty member and Associate Professor, Department of Pathology at the University of Pittsburgh, commended Dr. Yates and noted her dedication to mentoring in his letter of nomination: “She is an outstanding mentor because she listens, cares, and gives excellent advice. She always seems to know the best action to take now and how to prepare for the future…she is especially interested in helping to support traditionally underrepresented individuals in science, particularly women.”
Congratulations, Dr. Yates!
Dr. Dan Ding Awarded Grant for New Course

Dan Ding, PhD (pictured), McGowan affiliated faculty and Associate Professor in the Department of Rehabilitation Science at the University of Pittsburgh, is one of four faculty members chosen to receive the provost’s and Center for Teaching and Learning’s Open Online Short Course Development Grant.
The $10,000 grant was open to all full- and part-time faculty members and asked applicants to develop non-credit, stand-alone, asynchronous courses designed to serve large enrollments for the Coursera platform. The Coursera platform reaches more than 100 million learners globally.
Professor Ding’s course, titled “Harnessing the Potential of Smart Home Technology for Assistive Technology,” is intended to serve as a gateway to degree programs, either in-person or online, at the University.
Dr. David Gau Honored by Pitt’s Postdoctoral Association

David Gau, PhD (pictured), a third-year postdoctoral scholar in the Department of Bioengineering at the University of Pittsburgh, was honored by the Pitt Postdoctoral Association at the 16th Annual Postdoctoral Data and Dine Symposium. Dr. Gau, who is a member of McGowan affiliated faculty Dr. Partha Roy’s Cell Migration Lab, won the Postdoctoral Alumni Award.
The Data and Dine Symposium is a scientific poster session designed for postdoctoral fellows from across the University to showcase their research, as well as network and build connections with Pitt faculty and administrators.
Over 300 poster presenters and guests attended Data and Dine in Alumni Hall in the Connolly Ballroom, making this year’s event the largest in the Symposium’s history.
The Symposium honored Dr. Gau for his long-standing track record of representing various trainees at the University, including serving as the President of the University of Pittsburgh Postdoctoral Association (UPPDA) from 2019-2022.
During his tenure, Dr. Gau transformed the shared governance system at Pitt by successfully advocating for postdoc representation. This led to greater understanding about the postdoctoral population at the University and created more communication between postdocs and senior administration at Pitt. Dr. Gau also laid the foundation for improving benefits available to postdocs and standardizing postdoc salary to NIH standards. As a lecturer in the Department of Bioengineering and a member of the ad hoc Dependent Care Committee, Dr. Gau’s work advocating for postdocs continues.
The Postdoctoral Alumni Award is in recognition of Dr. Gau’s contributions to the Postdoctoral Association.
Congratulations, Dr. Gau!
Read more from the University Times and the Data and Dine Brochure.
PUBLICATION OF THE MONTH
Author: Raphael J. Crum, Kelsey Hall, Catalina Pineda Molina, George S. Hussey, Emma Graham, Hongshuai Li & Stephen F. Badylak
Title: Immunomodulatory matrix-bound nanovesicles mitigate acute and chronic pristane-induced rheumatoid arthritis
Summary: Rheumatoid arthritis (RA) is an autoimmune disease characterized by chronic inflammation and destruction of synovial joints affecting ~7.5 million people worldwide. Disease pathology is driven by an imbalance in the ratio of pro-inflammatory vs. anti-inflammatory immune cells, especially macrophages. Modulation of macrophage phenotype, specifically an M1 to M2, pro- to anti-inflammatory transition, can be induced by biologic scaffold materials composed of extracellular matrix (ECM). The ECM-based immunomodulatory effect is thought to be mediated in part through recently identified matrix-bound nanovesicles (MBV) embedded within ECM. Isolated MBV was delivered via intravenous (i.v.) or peri-articular (p.a.) injection to rats with pristane-induced arthritis (PIA). The results of MBV administration were compared to intraperitoneal (i.p.) administration of methotrexate (MTX), the clinical standard of care. Relative to the diseased animals, i.p. MTX, i.v. MBV, and p.a. MBV reduced arthritis scores in both acute and chronic pristane-induced arthritis, decreased synovial inflammation, decreased adverse joint remodeling, and reduced the ratio of synovial and splenic M1 to M2 macrophages (p < 0.05). Both p.a. and i.v. MBV reduced the serum concentration of RA and PIA biomarkers CXCL10 and MCP-3 in the acute and chronic phases of disease (p < 0.05). Flow-cytometry revealed the presence of a systemic CD43hi/His48lo/CD206+, immunoregulatory monocyte population unique to p.a. and i.v. MBV treatment associated with disease resolution. The results show that the therapeutic efficacy of MBV is equal to that of MTX for the management of acute and chronic pristane-induced arthritis and, further, this effect is associated with modulation of local synovial macrophages and systemic myeloid populations.
Source: NPJ Regen Med. 2022 Feb 2;7(1):13.
GRANT OF THE MONTH
PI: Julie Phillippi
Co-PI: Amrinder Nain
Title: Matrix biophysics and pericyte mechanobiology in (patho)physiological angiogenesis
Description: The long-term arc of this project is expected to engineer vascularization of tissue deficits and advance treatment of microvascular diseases including myocardial infarction, atherosclerosis, pulmonary arterial hypertension, aneurysm, peripheral artery disease, bone repair, volumetric muscle loss, diabetic wounds, and cancer. To achieve this goal, the project will advance our fundamental understanding of how local fibrous extracellular matrix (ECM) biophysical cues dynamically influence pericytes during neovessel formation. The role of the endothelial cell in vasculogenesis and angiogenesis is well recognized, yet the pericyte’s full scope of work is less understood, despite its known essential role in proper vascular development. We made a surprising observation that pericytes exhibit phenotypic plasticity when they spontaneously assemble into 3D spheroids and reversibly form and adopt endothelial markers when cultured on native and synthetic fibrous biomaterials in vitro, but not on 2D substrates. Akin to vasculogenic blood islands, tip cell-like protrusions sprout and retract from these spheroids comprised of pericytes that transdifferentiate to express endothelial markers. Other studies by our team revealed that matrix fiber diameter and architecture dictate cell morphology, the mode and rate of cell migration, cell force exertion, protrusion dynamics, and nuclear shape associated with heterochromatic rearrangements. These published and preliminary studies gave rise to a central hypothesis that various matrix biophysical parameters differentially direct neovessel formation by modulating pericyte migration, contraction, protrusion, and phenotypic plasticity. To test this hypothesis, we will further develop a nanofiber cell force sensing platform to mimic (patho)physiological ECMs through exquisite tunable control of ECM fiber biophysical parameters (e.g., diameter, density, alignment). With consideration of disease-simulating biochemical milieu (e.g., oxygen tension, reactive oxygen species, and inflammatory cytokines), experiments performed under Aim 1 will identify how matrix biophysical cues alter pericyte migration, contractility, and protrusion dynamics. Aim 2 experiments will develop the in vitro nanofiber scaffold system to selectively transplant patterned spheroids in vivo for neovessel formation through engineered control of pericyte plasticity and transdifferentiation. The project’s translational impact will be novel methods of controlling microvascular expansion and regression in diseased, damaged, and engineered tissues.
Source: National Heart, Lung, and Blood Institute
Term: May 5, 2023 – April 30, 2027
Amount: $581,795
