February 2018 | VOL. 17, NO. 2| www.McGowan.pitt.edu
Engineering a Functional Whole Organ for Transplantation
Per the United Network for Organ Sharing, every ten minutes, someone is added to the national transplant waiting list in need of a kidney, liver, pancreas, heart, lung, or intestine, the most needed organs of 2017. As of the end of January 2018, there were 114,883 people needing a lifesaving organ transplant (total waiting list candidates) with 74,722 of those people being active waiting list candidates. Tragically, on average, 20 people die each day while waiting for a transplant. More than 7,000 candidates died in 2016 while on the wait list, or within 30 days of leaving the list for personal or medical reasons, without receiving an organ transplant.
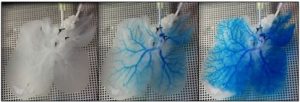
In the laboratory of McGowan Institute for Regenerative Medicine deputy director, Stephen Badylak, DVM, PhD, MD, professor in the Department of Surgery and director of the Center for Pre-Clinical Tissue Engineering within the Institute, researchers are working to increase the shortage of viable, transplantable livers by engineering a functional whole organ for treatment of end stage liver disease. Dr. Badylak and his team are aggressively investigating a therapeutic whole organ replacement strategy that is based upon the concept that functional hepatic tissue can be engineered by the effective delivery of autologous hepatic parenchymal and non-parenchymal cells within a xenogeneic 3-dimensional scaffold composed of liver extracellular matrix (3D L-ECM). This approach would include immediate in-situ transplantation of the cell seeded scaffold, providing the requisite perfusion by the host circulation that supplies appropriate microenvironmental cues, nutrients, and signaling factors necessary for liver regeneration.
By decellularizing the entire organ, most of the 3D structure of the extracellular matrix (ECM) can be retained to provide a native framework for organ reconstruction. The long-term goal of this work is to establish the decellularization, recellularization, and transplantation criteria necessary to produce a fully functional bioengineered liver for organ transplantation and drug discovery.
As Dr. Badylak explained to reporter Patrick J. Kiger, HowStuffWorks, “Success by this method means that the recipients would no longer be relegated to immunosuppressant therapy and would not have to wait for a matched donor organ.”
According to Dr. Badylak, more than a dozen scientific teams around the world are working to develop the ability to grow transplant organs from stem cells, in addition to other researchers who are working on the problem on a smaller scale. The most promising approach is decellularization, a technique in which the cells are stripped from a donor organ — usually one from a pig — leaving behind a tissue scaffold upon which the organ can be rebuilt by using stem cells, he says.
Illustration: Snapshots of blue dye flowing through the vasculature of a 3D rat liver ECM scaffold. Badylak Laboratory.
RESOURCES AT THE MCGOWAN INSTITUTE
March Histology Special
Come and see what the McGowan Histology Core has to offer. From Optic nerves to whole eye sectioning, we can give you what you’re looking for.
Bring your nerve tissue to the lab for Silver Staining for nerve fibers, Luxol Fast Blue for myelin, Cresyl Echt Violet stain for Nissl Substance, Tunel staining for apoptosis.
For the entire month of March you will receive 25% your entire bill when you bring your nervous system studies for histologic processing to the McGowan Histology Lab.
Contact Lori at the McGowan Core Histology Lab and ask about our staining specials by email or call 412-624-5265. As always, you will receive the highest quality histology in the quickest turn-around time.
Did you know the more samples you submit to the histology lab the less you pay per sample? Contact Lori to find out how!
EVENTS
 Regenerative Medicine Summer School 2018
Regenerative Medicine Summer School 2018
This year marks the 5th Annual McGowan Institute for Regenerative Medicine Summer School. This program is open to undergraduate students from all backgrounds, and serves as an in-depth introduction to regenerative medicine. Students attend lectures and have the opportunity to interact with more than 20 faculty, spanning highly diverse disciplines including basic science, engineering, medicine, clinical translation, and university start-ups and established biomedical industry. Students also participate in hands-on laboratory activities within the laboratories of the McGowan Institute, participate in networking opportunities, and visit multiple Pittsburgh sites. This year, there will also be 8-10 week paid internships available for interested students. Students will participate in the week-long Summer School program, and then continue to perform deeper research with a faculty member of the McGowan Institute. We hope that these opportunities will spur interest in the field of regenerative medicine and result in increased participation of students from diverse backgrounds. Interested students should visit http://www.mirm-pitt.net/professional-development/summer-school/. Faculty interested in hosting a student should contact Dr. Bryan Brown at brownb@upmc.edu.
SCIENTIFIC ADVANCES
Study of How Brain Interprets Visual Cues Could Aid Treatment of Psychiatric Disorders
 For people living with attention deficit disorder, their struggles are not a matter of refusing to pay attention for a long period of time.
For people living with attention deficit disorder, their struggles are not a matter of refusing to pay attention for a long period of time.
Instead, it might be that these people have difficulty monitoring their own attention — and maintaining it — so they can stay on task.
At least, that’s a hypothesis a Pittsburgh-based research duo wants to study by looking at the brain’s interaction with visual stimuli.
Their research aims to show how the sensory environment and a person’s mental state at a specific point in time combine to affect perception and interpretation of the outside world.
“We have the ability to tap into that state of mind with our approach and see if we can better understand how our perception works when we take the state of mind into account,” said McGowan Institute for Regenerative Medicine affiliated faculty member Matthew Smith, PhD, associate professor of ophthalmology at the University of Pittsburgh School of Medicine.
Dr. Smith and Byron Yu, PhD, an associate professor of electrical and computer engineering and biomedical engineering at Carnegie Mellon University, will use brain-computer interfaces to observe visual neurons — nerve cells that receive signals traveling from the eyes.
“Our goal is to show what these types of brain-computer interfaces can achieve outside of the motor system,” Dr. Smith said. “We’re trying to test the limits of what we can modify in our neural activity. We can try to teach our subjects how to control their own internal state.”
So, what does perception have to do with paying attention in class or at work? Dr. Smith said attention is one of the most well-known internal states that affects perception.
“If we pay attention or not, it can cause us to notice or miss important details in the world,” he said. “We try to teach the subject to directly access the internal states.”
Dr. Smith said this is an important approach, because many psychiatric, neurological and behavioral disorders like attention deficit disorder arise from problems in controlling internal states, rather than problems in sensory processes, like a retinal problem in the eye.
Drs. Smith and Yu have collaborated before, but this study merges both researchers’ backgrounds and focuses, with Dr. Smith’s area of specialty being in electrophysiology and experimentation and Dr. Yu’s expertise in brain-computer interfaces and computational approaches.
One place of inspiration for their study comes from an unlikely source: people who are paralyzed and are able to move cybernetic limbs through thinking.
“When they think about moving, even though they can’t actually move, it is possible to listen in to their motor neurons and use that to guide a computer cursor or a robotic arm,” Dr. Smith said.
Dr. Smith said the project takes the idea that thinking can lead to physical movement in robotic or computer-based systems and applies it to the sensory and cognitive domains. If successful, it may aid in treatment of more cognitive disorders such as attention deficit disorder and in recovery of function after brain injury.
To accomplish this, the researchers will try to make animals control their brains in a way that maximizes their attention.
“We teach animals to expect a visual stimulus, like a flash, that will appear at a certain location in space,” Dr. Smith said. “We can show through their behavior that they’re paying attention to the visual flash and listen in on their neurons at the same time. Then, we can build an interface to give them feedback and observe how it affects their attention.”
These target trainings offer hope that in the future, people may be able to be taught how to focus more in an academic environment and in daily life.
Pitt Researchers Look at “Relaxin” to Heal an Aging Heart
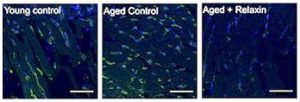
As we age, the risk of developing cardiovascular disease such as heart failure and atrial fibrillation increases dramatically, and the rates of these age-associated diseases are expected to rise with a rapidly aging population. A team of researchers at the University of Pittsburgh believes that a naturally occurring hormone, relaxin, can reverse some of the effects of aging on the heart to reduce these risks through inhibiting a chronic, age-associated inflammatory response termed “inflammaging”.
The study was led by McGowan Institute for Regenerative Medicine affiliated faculty member Guy Salama, PhD, professor of medicine at Pitt, and Brian Martin, his graduate student researcher from the Swanson School of Engineering’s Department of Bioengineering.
“While inflammation is helpful in instances of tissue injury or infection, the inflammatory response usually subsides upon injury resolution,” Mr. Martin explains. “However, in aging, there appears to be low-grade, systemic inflammation which can result in excess inflammatory and immune cells producing substances that are toxic to surrounding tissue.”
In the case of the heart, damage to nearby tissue leads to pathological remodeling that lowers the threshold for disease development. “A notable occurrence in many cardiovascular diseases is a natural response to injury where collagen builds up on or between cells,” said Mr. Martin. “This accumulation can cause the heart to function improperly.”
Relaxin is a naturally occurring hormone in the body that was discovered for its involvement in pregnancy and childbirth; however, studies have shown that it has multiple benefits outside of pregnancy in both sexes.
“In a study using a male rat model of aging we showed that relaxin dramatically reduced incidence of arrhythmias, which can lead to stroke and sudden death,” said Dr. Salama. “We then found that relaxin reversed maladaptive electrical changes that are known to occur in patients with atrial fibrillation. Its primary effects were a dramatic reduction in collagen accumulation and a beneficial remodeling of cardiac electrical components needed for proper heart contraction.”
“While much work is being done to understand how relaxin leads to these changes, the mechanisms by which relaxin mediates its effects are still largely unknown,” said Mr. Martin.
“We used RNA-sequencing to count the messenger RNA (mRNA) levels in the tissue so that we can gauge what aging is doing at the genetic level and if relaxin can reverse these effects,” said Mr. Martin. “We then used a computational approach to analyze the differences in gene expression patterns of the rats and examined the vast literature on what each gene may be involved in. This can begin to predict what functional effects these genes will have in the body.”
The results showed a difference in inflammatory and immune signaling between the male and female rats. The female rats had an overexpression of inflammatory and immune related genes which upon relaxin treatment, were suppressed. Though male rats did not show activation of inflammatory or immune responses in aging, relaxin still reduced gene expression of many inflammatory-related genes. These data suggest that relaxin can act as a potent anti-inflammatory.
The team plans to continue research to further understand the effects of relaxin on “inflammaging.” “These results open a multitude of exciting possibilities,” said Dr. Salama. “Many cardiovascular diseases have an associated inflammatory component, and therefore, relaxin could be a potential therapy for these diseases.”
A 3-D Approach to Stop Cancer in Its Tracks
Every day, roughly 100 billion new cells are created inside the human body. These cells join trillions of older cells to form the tissues and organs we rely on to stay alive. Sometimes when a cell is created, a mutation occurs within its DNA, transforming the cell into something defective and potentially dangerous to the body’s internal environment. Usually, a cell will recognize its own defects and quickly terminate itself.
But sometimes, instead of eliminating itself, the mutated cell replicates, forming a tumor that could break apart, metastasize (i.e. migrate), and invade other parts of the body—oftentimes through the bloodstream. Fortunately, McGowan Institute for Regenerative Medicine affiliated faculty member and Carnegie Mellon University Mechanical Engineering (MechE) Professor Philip LeDuc, PhD, in collaboration with mechanical engineering PhD student James Li Wan and Carola Neumann, MD, a breast cancer researcher from the University of Pittsburgh, developed a patient-oriented model scientists can use to better understand—and eventually stop—cancer cell migration. The study was recently published in Scientific Reports.
According to Dr. LeDuc, this project began because of the growing interest researchers have shown in the relationship between physical science and cancer. Since tumors are actually physical masses, both biochemical and physical means can affect cancer cells and tumors. After considering the connection between these two topics, Drs. LeDuc, Neumann, and Mr. Wan turned their attention to metastasis and cancer cell analysis. Through their collaboration, they were able to develop a more accurate and relevant way to study cancer cells.
Although cell analysis traditionally occurs in a plastic petri dish, the research team created a 3-D model that more accurately reflects the physiological conditions of an organism. With this model, scientists can uncover and analyze the complexities of cancer cells in an environment that more closely mimics the human body.
“Biology has been studied by putting cells inside of petri dishes for decades,” says Dr. LeDuc. “But the question is, can you make systems that are more physiologically relevant? We’re using microfluidic and microfabrication approaches to create three dimensional systems because cells exist in three dimensional tissues—they don’t naturally reside in a 2-D petri dish.”
Typically, microfluidic systems—systems that transfer liquids at the microscopic level—are made of plastic, but since Drs. LeDuc, Neumann, and Mr. Wan were searching for a more physiologically relevant system, they created their microfluidic system using collagen, the most predominant protein in the human body.
“As Phil said, we traditionally grow cells in plastic and work with them in petri dishes,” says Dr. Neumann, an associate professor of pharmacology and chemical biology at the University of Pittsburgh. “But nowhere in your body do you have plastic. Having a 3-D system that mimics physiological conditions is a much better way to get faster and more relevant results.”
Each microfluidic device created by the team contains two key components: a set of parallel channels that mimic traditional blood vessels and a concentration of cancer cells that are embedded in the collagen.
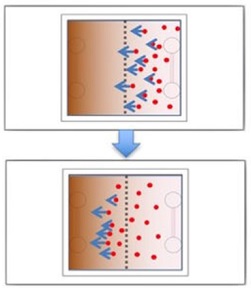
Once a device is constructed, the channels are injected with a chemical stimulant that diffuses into the surrounding collagen. As molecules from the stimulant move further away from the channels, a biomolecular gradient is created. This gradient prompts the embedded cancer cells to move—often back toward the simulated blood vessel channels.
In a patient, if cancer cells enter the bloodstream, they metastasize and can form secondary cancer tumors. According to Drs. LeDuc and Neumann, most patients with solid tumors usually die from metastasis—not from the primary tumor itself—which is why scientists must figure out how to stop metastasis from occurring in the first place.
Metastasizing cancer cells have acquired the ability to move from the primary tumor into the blood or lymph system—a process that requires cancer cells to migrate and remodel the tumor tissue to invade other parts of the body. So, in order to stop metastasis, scientists need to understand which factors support cancer cell mobility and tissue remodeling. This is why the 3-D system developed by Drs. LeDuc, Neumann, and Mr. Wan is so important.
“Cancer is an extremely heterogeneous disease, which means that not only do cancer cells differ from patient to patient, they vary even within one tumor,” says Dr. Neumann. “The same is true for metastases. Depending on their location in the body, each additional secondary tumor is different as well.”
To determine the best treatment for each patient, Drs. LeDuc, Neumann, and Mr. Wan believe that researchers will eventually be able to use their system to examine tumors from individual cancer patients. This process would ultimately help make cancer treatment more personalized and effective.
“Our model could potentially serve as a patient-specific model,” says Mr. Wan, who conducted the lab experiments and analyzed the results for this study. “And that’s very important because cancer is different in each patient, which makes it hard to cure.”
Ideally, the 3-D system developed by the team will give researchers and scientists the tools they need to stop cancer cells from metastasizing in every patient.
“At the end of the day, the tumor that’s sitting there and doing nothing—that’s okay,” says Dr. LeDuc. “But as soon as it goes metastatic, everything breaks loose. We hope that our system will help stop metastasis and improve patient outcome in the long run.”
Illustration: Experimental design and confocal imaging with MDA-MB-231 cancer cells initially located in the right half of system. The cells migrate to the left due to the FBS gradient. Scientific Reports.
Vascular Bypass Grafting: A Biomimetic Engineering Approach
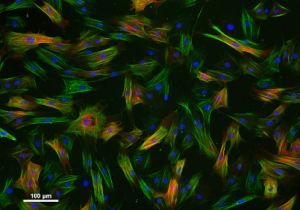
When a patient with heart disease is in need of a vascular graft but doesn’t have any viable veins or arteries in his or her own body, surgeons can rely on synthetic, tissue-engineering grafts. However, the body often treats these substitutes as a threat and rejects them. Researchers at the University of Pittsburgh are developing synthetic grafts that mimic the body’s own blood vessels to mitigate many of the complications of bypass surgery.
“The current best available treatment is to use the patient’s saphenous vein or mammary artery, but not everyone has enough of these healthy blood vessels to use when they need a bypass,” says McGowan Institute for Regenerative Medicine affiliated faculty member Jonathan Vande Geest, PhD, Professor of Bioengineering at Pitt’s Swanson School of Engineering. “A biocompatible, tissue-engineered graft would provide these patients with treatment options that currently do not exist.”
The National Institutes of Health awarded Dr. Vande Geest and his multi-institutional research team $672,682 for his one-year study, “Preclinical assessment of a compliance matched biopolymer vascular graft.” His research builds upon his work at Pitt’s Soft Tissue Biomechanics Laboratory designing newly engineered materials that mechanically and microstructurally behave the same way as the body’s native tissues.
“‘Biomimetic’ means that we study the organization and architecture of normal healthy tissue and use this information to guide our design and development of a tissue-engineered substitute,” explains Dr. Vande Geest. “For example, every functioning artery has a one-cell thick lining called an endothelium responsible for reducing thrombosis and controlling blood flow. Our graft will be endothelialized using blood derived endothelial cells.”
Large-diameter vascular grafts are commonly used in some vascular surgeries and can function perfectly up to 10 years after implantation. However, the body often treats small-diameter grafts as dangerous foreign objects. The result can be artery occlusion or blood clotting—detrimental conditions called hyperplasia and thrombosis, respectively.
“Small-diameter vascular grafts, or grafts involving blood vessels with an internal diameter smaller than five millimeters, have much higher failure rates than larger ones,” says Dr. Vande Geest. “A significant proportion of vascular disease cases involve small-diameter blood vessels, so the demand for viable treatment options is very high.”
A normal healthy artery is organized with alternating layers of collagen and elastin, which provide structural support and elasticity. Dr. Vande Geest’s proposed graft uses alternating layers of gelatin and tropoelastin as substitutes. Gelatin is derived from collagen, and tropoelastin is a precursor to elastin. He will use these materials along with computational optimization to engineer a graft with compliance similar to a real artery, eliminating compliance mismatch – an important rejection mechanism in currently used grafts.
“We believe our method of mimicking native artery microstructure and mechanics will result in a successful tissue-engineered graft, and this grant will support trials to perfect both our experimental and computational approach,” says Dr. Vande Geest.
Illustration: Vascular smooth muscle cells.
McGowan Institute Affiliated Faculty Projects Receive Pitt’s Center for Medical Innovation Awards Round-2 2017 Pilot Funding

The University of Pittsburgh’s Center for Medical Innovation (CMI) awarded grants totaling $115,000 to five engineering and medicine groups through its 2017 Round-2 Pilot Funding Program for Early Stage Medical Technology Research and Development. Four of the five projects are led by McGowan Institute for Regenerative Medicine affiliated faculty members. The latest McGowan Institute faculty funded proposals include proposed solutions to conditions such as peripheral artery disease, pulmonary fibrosis, improved wound healing and repair, and a better means to perform root canal surgery.
The Center for Medical Innovation, a University Center housed in Pitt’s Swanson School of Engineering, supports applied technology projects in the early stages of development with “kickstart” funding toward the goal of transitioning the research to clinical adoption. Proposals are evaluated on the basis of scientific merit, technical and clinical relevance, potential health care impact and significance, experience of the investigators, and potential in obtaining further financial investment to translate the particular solution to healthcare.
“We have an extremely strong cohort from our 2017 Round 2 funding,” said McGowan Institute affiliated faculty member Alan Hirschman, PhD, CMI Executive Director. “The collaboration between engineering and medicine at Pitt provides a fertile setting for novel medical technology, and so we’re proud to give these researchers funding to take their ideas to the next level.”
The funded projects include:
A Structurally and Mechanically Tunable Biocarpet for Peripheral Arterial Disease
Development of a prototype “Biocarpet” that is mechanically and topographically tunable and can be used to treat complex peripheral artery disease. This will help treat long lesions in peripheral arteries that have multiple stenoses.
Jonathan Vande Geest, PhD, Professor of Bioengineering, University of Pittsburgh Swanson School of Engineering
Kang Kim, PhD, Associate Professor of Medicine, University of Pittsburgh School of Medicine; and secondary appointment in Departments of Bioengineering and Chemical Engineering, University of Pittsburgh Swanson School of Engineering
William Wagner, PhD, Professor of Surgery University of Pittsburgh School of Medicine; Director, McGowan Institute, and secondary appointments in Department of Bioengineering, University of Pittsburgh Swanson School of Engineering
John Pacella, MD, MS, Assistant Professor of Medicine, Division of Cardiology, University of Pittsburgh School of Medicine; and Vascular Medicine Institute
Kenneth Furdella, Graduate Student, Department of Bioengineering, University of Pittsburgh Swanson School of Engineering
FibroKine: CXCL10 Biomimetic Peptides for Treatment of Pulmonary Fibrosis
Development of an inhaled aerosol delivery system will achieve target organ specificity and efficient delivery to the lung. This will specifically aid patients who suffer from pulmonary fibrosis.
Cecelia Yates, PhD, Assistant Professor of Health Promotion and Development, University of Pittsburgh School of Nursing
Timothy Corcoran, PhD, Associate Professor of Medicine, Division of Pulmonary, Allergy, and Critical Care Medicine, University of Pittsburgh School of Medicine; and secondary appointments in departments of Bioengineering and Chemical and Petroleum Engineering, University of Pittsburgh Swanson School of Engineering
Zariel Johnson, PhD, Postdoctoral Associate, Department of Health Promotion and Development, University of Pittsburgh School of Nursing
Christopher Mahoney, MS, PhD Candidate, Department of Bioengineering, University of Pittsburgh Swanson School of Engineering
Gel-Based Reconstructive Matrix for Treating Orbital Trauma and Periocular Wounds
Development of a novel ocular trauma management system, for immediate response to injuries that occur to the areas including and surrounding the eye.
Morgan Fedorchak, PhD, Assistant Professor of Ophthalmology and Clinical & Translational Sciences, University of Pittsburgh School of Medicine; secondary appointment in Chemical Engineering, University of Pittsburgh Swanson School of Engineering; and Louis J. Fox Center for Vision Restoration
Jenny Yu, MD, FACS, Assistant Professor and Vice Chair for Clinical Operations Department of Ophthalmology, UPMC Eye Center; and Assistant Professor of Ophthalmology and Otolaryngology, University of Pittsburgh School of Medicine
Michael Washington, PhD, Postdoctoral Scholar, Department of Ophthalmology, University of Pittsburgh School of Medicine
Vital-Dent, a Revitalizing Root Canal Solution
Development of a novel device to regenerate vital tooth pulp after root canal therapy. Vital pulp will help protect the tooth from future infection and injury, reducing the need for tooth extraction, implants, and dentures.
Juan Taboas, PhD, Department of Oral Biology, University of Pittsburgh School of Dental Medicine; secondary appointment, Department of Bioengineering, University of Pittsburgh Swanson School of Engineering; and Center for Craniofacial Regeneration
Herbert Ray Jr., DMD, Assistant Professor of Endodontics and Director, Graduate Endodontic Residency Program, University of Pittsburgh School of Dental Medicine; and Center for Craniofacial Regeneration
Jingming Chen, BS, Department of Bioengineering, University of Pittsburgh Swanson School of Engineering; and Center for Craniofacial Regeneration
Congratulations, all!
Illustration: Center for Medical Innovation.
Dealing with Diastasis Recti

Diastasis recti is a non-life-threatening condition affecting the pair of long, flat muscles, known as the rectus abdominis, that run vertically down each side of the abdomen. These muscles are referred to as “six-pack muscles” and help stabilize the body’s trunk and hold in the abdomen’s internal organs. Mostly affecting women, diastasis recti happen when these muscles separate, often during pregnancy or after giving birth, leaving a gap, a belly pouch, or a sense of abdominal weakness.
Other health issues that may arise due to a diastasis include chronic low back pain, pelvic or hip pain, constipation, urinary incontinence, and pain during sex. Specialized physical therapy can help reduce this unwelcome change and regain strength in these muscles. If the diastasis is severe and there are no plans to get pregnant again, surgery may be an option.
McGowan Institute for Regenerative Medicine affiliated faculty member Kenneth Shestak, MD, Chief of Plastic Surgery at Magee-Womens Hospital of UPMC and Professor of Surgery in the Division of Plastic and Reconstructive Surgery, University of Pittsburgh School of Medicine, cares for patients with diastasis recti and recently spoke with Pittsburgh KDKA reporter Heather Abraham about the condition and its treatment options.
With specialized physical therapy, “There are five paired muscles that work together and if you can strengthen the muscles many times you can see an improvement in that separation,” Dr. Shestak said. “What we tend to see are people who’ve really worked hard to try to do it without surgery and still have a bulge in the mid-portion of the abdomen.”
He also noted that moms are not the only ones who suffer from this. Dr. Shestak said he sees it frequently in patients who’ve gained a lot of weight and sometimes in men who do a lot of weight lifting.
While the condition is not life-threatening, it’s not something you want to let go.
“If left to its own devices and it progresses, there can be problems with back pain, discomfort when getting out of a chair, arising from a sitting position to a standing position,” Dr. Shestak said.
For people who do have to have surgery for this, Dr. Shestak said recovery time is fairly quick these days thanks to advancements in how they do the operation. He said the procedure not only treats the underlying muscle problem, but also helps improve the shape and contour of the abdomen.
Wearable Artificial Lung Designed to Help Sick Children Remain Mobile While Hospitalized

Artificial lungs have long been used to help sick children until a lung transplant is available.
While these devices are helpful in supplying oxygen to children suffering from cystic fibrosis, pulmonary hypertension, and pulmonary fibrosis, among other diseases, during the wait for lung transplants, they restrict mobility.
“They are labor intensive, there is a lot of equipment involved, and they essentially keep these kids bedridden,” said McGowan Institute for Regenerative Medicine faculty member William Federspiel, PhD, the William Kepler Whiteford Professor in the University of Pittsburgh Swanson School of Engineering Department of Bioengineering.
At Pitt, Dr. Federspiel has been researching ways to create a more compact respiratory assistance device for children. The work has been fruitful, with the Pittsburgh Pediatric Ambulatory Lung (PPAL) aiming to serve as a bridge to transplantation or recovery in children with acute and chronic lung failure.
This wearable artificial lung, half the size of a coffee can, will be designed for longer-term respiratory support, about one to three months before device change-out. The device will supply between 70 and 90 percent of normal metabolic oxygenation requirements, while pumping blood from one to 2.5 liters per minute.
Perhaps most importantly though, the device will help pediatric patients get out of bed and engage in activity as soon as possible after an operation.
Studies have shown that ambulation during the waiting period for lung transplantation significantly improves post-transplant outcomes.
“Patients won’t be going home with the technology,” said Dr. Federspiel. “But it will allow them to move about in a hospital setting.”
An adult version of the lung is also in the works.
Dr. Federspiel said the next step for the artificial lung is to find ways to further translate the project toward clinical use.
“The number of pediatric patients is very small, and because the expense of going through the regulatory processes is a burden, it can be difficult to commercialize pediatric technologies like this,” he said.
The researchers are working with the McGowan Institute for Regenerative Medicine and Children’s Hospital of Pittsburgh of UPMC’s Pediatric Device Initiative, in collaboration with sciVelo, to help advance the commercial translation.
“The idea is to be able to bring to patients in lung failure the technologies now available to patients in heart failure, to have technology that gives patients the quality of life where they’re able to be mobile and not be tethered in the intensive care unit,” said William Wagner, PhD, director of the McGowan Institute. “We’re trying to make these devices biocompatible, so they don’t form blood clots.”
The project was recently awarded a four-year, $2.9 million grant from the National Institutes of Health. Along with co-PIs Drs. Federspiel and Wagner, McGowan Institute faculty member Peter Wearden, MD, PhD, congenital cardiothoracic surgeon and Department Chair, Division of Cardiovascular Surgery, Department of Cardiovascular Services at the Nemours Children’s Health System, Orlando, Florida, is a co-PI on the NIH grant.
Collaboration to Innovation
The Pediatric Device Initiative (PDI) is a McGowan Institute for Regenerative Medicine initiative in collaboration with Children’s Hospital of Pittsburgh of UPMC that aims to transform pediatric health care through the advancement of novel treatments for pediatric tissue and organ failure. The initiative has partnered with sciVelo to assist in accelerating the translation of novel pediatric technologies.
sciVelo is a University of Pittsburgh commercial translation program born out of the Schools of the Health Sciences in 2016.
At Pitt, sciVelo works to support a collaborative and efficient commercial translation ecosystem, leveraging local and national translational resources, to establish Pittsburgh as a gold standard for accelerating early stage research investigators to high impact translational outcomes.
The Pittsburgh Pediatric Ambulatory Lung was among the first cohort of initiative-funded projects. Its conception was a direct result of the initiative’s core partnership between the McGowan Institute and Children’s Hospital.
“The relevancy to convey the initiative’s ability to build momentum for pediatric innovation is not only exciting for children’s health care, but also the Pittsburgh region,” said McGowan Institute affiliated faculty member Donald Taylor, MBA, PhD, assistant vice chancellor for commercial translation in the health sciences and sciVelo executive director. “The progress in development and translation of this revolutionary project is a product of the culture of pediatric innovation in the health sciences, established and fostered by the initiative.”
Along with the artificial lung, the initiative also directly funds several other early stage pilot projects aimed toward pediatric patients.
Illustration: A wearable artificial lung will help pediatric patients get out of bed and engage in activity as soon as possible after an operation.
New Gordon Research Conference on Neuroelectronic Interfaces Co-Founded by Dr. Takashi Kozai
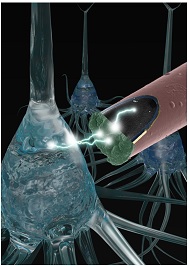
McGowan Institute for Regenerative Medicine affiliated faculty member Takashi Kozai, PhD, assistant professor of bioengineering at the University of Pittsburgh Swanson School of Engineering, will act as co-vice chair at the inaugural Gordon Research Conference on Neuroelectronic Interfaces. The meeting will take place March 25-30, 2018 in Galveston, Texas.
Neuroelectronic interfaces—commonly known as brain-machine (or brain-computer) interfaces—create a direct communication line from the central nervous system to the outside world. This connection allows scientists to research ways to rehabilitate those with paralysis, other forms of motor dysfunction, or limb loss.
“One major limitation for practical clinical translation, despite nearly 60 years of chronic neural interface research, is that there remains a poor understanding of the complex biological and material failure modes across all classes of microelectrode arrays,” Dr. Kozai explains. “Among several classes of multi-modal problems encountered, the strong foreign body response, scar tissue formation, and implant material breakdown over time are critical obstacles. These issues ultimately lead to an electrical decoupling of implanted devices from the brain and a loss of signal.”
“Our inaugural Gordon Research Conference (GRC) on Neuroelectronic Interfaces will challenge the international field to turn back to the drawing board of basic materials research armed with emerging basic neurosciences knowledge,” Dr. Kozai says.
The event will bring together a multi-disciplinary team of leading experts in cellular neuroscience, brain pathology, neuro-technology, and materials science to discuss and eventually solve these challenges in order to achieve a chronically useful and reliable neural interface.
Dr. Kozai leads the Bio-Integrating Optoelectric Neural Interface & Cybernetics Lab (B.I.O.N.I.C. Lab) in the Swanson School of Engineering. The lab takes a multidisciplinary approach to better understand interactions at micro-scale neural interfaces and develop next-generation neural technologies that reduce or reverse negative tissue interactions.
“As both scientific knowledge and technological advances progress, we’re finding that many of the assumptions that were made in the field are limited in scope, or incomplete,” Dr. Kozai says. “As a result, we see more and more of these dogmas fall apart as we push the limits of engineering.”
See the research being done at Pitt’s Human Neural Prosthetics Program.
Illustration: Electrophysiological signals being detected from neurons (blue) with a sub-cellular sized implantable composite microelectrode designed to stealthily avoid the foreign body response. (Image by TDY Kozai/BionicLab.ORG)
AWARDS AND RECOGNITION
Dr. Flordeliza Villanueva Named Peter J. Safar Pulse of Pittsburgh Award Winner by American Heart Association

The 2018 Pittsburgh Heart Ball took place on February 17th at the Pittsburgh Wyndham Grand Hotel. 550 supporters came to celebrate the award recipients and raise $1.2 million for research and prevention of stroke and heart attack education.
This affair marks the presentation of the Peter J. Safar Pulse of Pittsburgh Award. This year the award was received by McGowan Institute for Regenerative Medicine affiliated faculty member Flordeliza Villanueva, MD.
Dr. Villanueva is currently Professor of Medicine in the Division of Cardiology and Vice Chair for Pre-Clinical Research of the Department of Medicine. In the clinical arena, Dr. Villanueva is the Director, Non-Invasive Cardiac Imaging, UPMC Heart and Vascular Institute, overseeing the clinical imaging programs in Echocardiography, Nuclear Cardiology, and Cardiac Magnetic Resonance. She has focused her research on the development of ultrasound contrast agents (microbubbles) for assessment of the microcirculation, ultrasound molecular imaging, and ultrasound-mediated therapeutics.
Dr. Villanueva is also the Director of the Center for Ultrasound Molecular Imaging and Therapeutics, UPMC Heart and Vascular Institute, a multidisciplinary translational research facility espousing the philosophy that moving technologies from pre-clinical status to the bedside requires strong traditional science and engineering, married to strong entrepreneurship. Her laboratory was the first to demonstrate that molecularly targeted microbubbles bind to biological surfaces overexpressing molecular targets, ultimately allowing ultrasonic imaging of disease/function-specific epitopes in vivo. Her group has led the study of how unique acoustic behaviors of microbubbles can be harnessed to therapeutic effect, such as drug/gene delivery or sonothrombolysis. She led the development of the UPMC Cam, an ultra-high speed microscopy imaging system capable of acquiring images at up to 25 million frames per second in either bright-field or fluorescence modes. Such a system allows the direct visualization of the mechanics of a single oscillating microbubble and the dynamics of a microbubble’s interaction with biological cells. This unique tool will help us better understand microbubble dynamics, mechanisms of microbubble mediated bioeffects, and improve their design for specific applications.
The American Heart Association – Allegheny Division board of directors and the Heart Ball committee created the Pulse of Pittsburgh Award in 2003 to recognize an individual’s leadership in the fight against heart disease and stroke. In 2004, the committee changed the name to the Peter J. Safar Pulse of Pittsburgh Award in honor of the late Peter J. Safar, MD, distinguished professor of resuscitation medicine at the University of Pittsburgh, who also was known as the Father of CPR.
Congratulations, Dr. Villanueva!
Illustration: American Heart Association.
Dr. Ron Poropatich Named Director of Pitt’s CMMR

McGowan Institute for Regenerative Medicine affiliated faculty member Ron Poropatich, MD, has been named the Director of the Center for Military Medicine Research (CMMR), Health Sciences, at the University of Pittsburgh. Dr. Poropatich (Professor of Medicine, Division of Pulmonary, Allergy and Critical Care Medicine; Senior Advisor for Telemedicine, UPMC; and retired US Army Colonel) has made significant inroads with senior leaders of the U.S. Department of Defense (DOD) medical research community and University of Pittsburgh faculty since his arrival at Pitt in 2012, when the Center was established.
The mission of the CMMR is to develop new research themes and to promote collaboration among investigators in the Health Sciences and related disciplines, which will lead to significant scientific and clinical advances that support the medical needs of the DOD and Veterans Affairs. Examples of novel medical research themes developed at Pitt and funded by the DOD include whole eye transplant, traumatic brain injury treatments, a trauma care research consortium in support of battlefield casualties, closed loop robotic controlled cardiopulmonary resuscitation, and human performance optimization. Dr. Poropatich’s active outreach across the Health Sciences has been exemplary and resulted in more than $100M in DOD funding over the last five years to 16 Pitt investigators. The Center’s efforts in other disciplines, such as regenerative medicine, reconstructive surgery, tissue engineering, and acute lung injury, have also been productive.
The Center has established an important network of successful partnerships and collaborations among scientists, clinicians, industry, the DOD, and the Veterans Administration. These relationships have led to strategic partnerships, promising research technologies, and emerging therapeutic strategies. With Dr. Poropatich’s determined leadership, the Center will continue to serve Pitt and facilitate research on health sciences and rehabilitation outcomes with the constant aim of accelerating the transition of innovative therapies to the military medical community. The Center has also provided an ideal multidisciplinary training environment that encourages students, trainees, and investigators to address the conceptual, methodological, and analytical issues implicit in advancing research for wounded members of the armed services.
Further, the Center has two additional McGowan Institute affiliated faculty members on the CMMR team:
- Michael R. Pinsky, MD (Professor of Critical Care Medicine) serving as Clinical Initiatives Advisor, and
- Bradley Nindl, PhD (Director of the Neuromuscular Research Laboratory/Wounded Warrior Human Performance Center and Professor of Sports Medicine and Nutrition in the School of Health and Rehabilitation Sciences as well as an Army Reservist Colonel commanding the Southwest Medical Area Readiness Support Group) serving as Senior Military and Scientific Advisor.
McGowan Institute faculty member Rocky Tuan, PhD, was founding Director of the CMMR and is now head of the Chinese University of Hong Kong.
Congratulations, Dr. Poropatich!
Regenerative Medicine Podcast Update
The Regenerative Medicine Podcasts remain a popular web destination. Informative and entertaining, these are the most recent interviews:
#180 –– Dr. Justin Weinbaum is a Research Assistant Professor in the Department of Bioengineering at the University of Pittsburgh. Dr. Weinbaum discusses his research on vascular tissue engineering.
Visit www.regenerativemedicinetoday.com to keep abreast of the new interviews.
PUBLICATION OF THE MONTH
Author: Wan L, Skoko J, Yu J, LeDuc PR, Neumann CA.
Title: Mimicking Embedded Vasculature Structure for 3D Cancer on a Chip Approaches through Micromilling
Summary: The ability for cells to sense and respond to microenvironmental signals is influenced by their three dimensional (3D) surroundings, which includes the extracellular matrix (ECM). In the 3D environment, vascular structures supply cells with nutrients and oxygen thus affecting cell responses such as motility. Interpretation of cell motility studies though is often restricted by the applied approaches such as 2D conventional soft lithography methods that have rectangular channel cross-sectional morphology. To better simulate cell responses to vascular supply in 3D, we developed a cell on a chip system with microfluidic channels with curved cross-sections embedded within a 3D collagen matrix that emulates anatomical vasculature more closely than inorganic polymers, thus to mimic a more physiologically relevant 3D cellular environment. To accomplish this, we constructed perfusable microfluidic channels by embedding sacrificial circular gelatin vascular templates in collagen, which were removed through temperature control. Motile breast cancer cells were pre-seeded into the collagen matrix and when presented with a controlled chemical stimulation from the artificial vasculature, they migrated towards the vasculature structure. We believe this innovative vascular 3D ECM system can be used to provide novel insights into cellular dynamics during multidirectional chemokineses and chemotaxis that exist in cancer and other diseases.
Source: Scientific Reports. 2017 Dec 1;7(1):16724.
GRANT OF THE MONTH
PI: Jonathan Vande Geest
Title: Preclinical assessment of a compliance matched biopolymer vascular graft
Description: Heart disease was responsible for 614,348 deaths in 2014, making it the leading cause of death for both women and men in the United States [1]. Over 400,000 coronary artery bypass graft (CABG) procedures were performed in 2010 alone, with reintervention rates reported to be as high as 8.8% [2]. In addition to limited autologous tissue availability, the treatment of small diameter vascular disease is hindered by the compliance mismatch of currently delivered grafts that lead to subsequent failure via intimal hyperplasia (IH) and graft thrombosis [3-7]. Despite significant recent progress, the development of a compliance matched and biologically functional TEVG has remained elusive. The utility of biopolymer based constructs have been promising [8], however there has been limited success in modulating the compliance and mechanical properties of these materials. Our overall hypothesis is that a TEVG composed primarily of alternating layers of gelatin and tropoelastin can be compliance matched to native tissue and, when lined with an autologous blood derived endothelium, reduce the current failure modes of small diameter vascular grafts. We further hypothesize that the elution of TGFβ2 from our graft will maintain the compliance of our TEVG following implantation. Therefore, the goal of this proposal is to assess the matrix remodeling, mechanical properties, thrombosis, and IH of our endothelialized, biomimetic, and compliance matched TEVG using both an in-vitro and in-vivo approach. This goal will be met by completing the following specific aims. Specific Aim 1: Fabricate a layered TEVG that is compliance matched to a rat aorta and an ovine carotid artery using our established experimental/computational optimization approach. Specific Aim 2: Determine the compliance, load dependent ECM organization, and protease activity of our cell seeded TEVGs as TGFβ2 is released during mechanically stimulated bioreactor culture. Specific Aim 3: Determine the compliance (in-vivo), patency, thrombogenicity, IH, and ex-vivo load dependent microstructure and mechanical properties of TGFβ2 eluting and compliance matched TEVGs. Specific Aim 4: Assess the patency, thrombogenicity, IH, and ex-vivo load dependent microstructure and mechanical properties of TGFβ2 eluting and compliance matched TEVGs lined with ECs derived from autologous adult versus autologous umbilical cord blood following ovine carotid implantation. Successful completion of the proposed aims will result in a TEVG that immunocompatible, antithrombogenic, and maintains it’s compliance matched mechanical properties following implantation. The proposed research will also generate novel information regarding the extracellular matrix remodeling of biopolymer based vascular grafts as they remodeled both in-vitro and in-vivo.
Source: NHLBI
Term: 9/26/2017 – 8/31/2018
Amount: $672,682
